Pneumonia refers to an infection that attacks the breathing system of a human being. It involves the air sacs of one or both lungs filling up with fluid or pus. Pneumonia can also be referred to as the lung parenchyma’s inflammation with alveolar edema and congestion that leads to impaired gas exchange.
It is a life-threatening infection, especially to infants, children, people who smoke, bed-ridden, malnourished, hospitalized, and people over sixty-five. The infection is airborne.
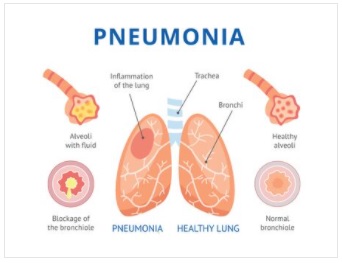
This means that its transmission mode is air through exposure to respiratory droplets, cough, saliva or sneezes, from an already infected person. Another cause of pneumonia is the inhalation of bacteria, viruses, and sinuses already existing in your nose directly into the lungs.
Read our popular article " Blood Oxygen Levels: What You Need to Know"
Nursing diagnosis for pneumonia
Diagnosis refers to the process of identifying a disease from its signs and symptoms.
Therefore, diagnosis for pneumonia refers to the process by which a nurse can conclude that a patient is suffering from pneumonia after identifying the signs and symptoms associated with it.
On the other hand, the prognosis refers to an opinion, most based on medical experience or past experience that tells the most likely course of a medical condition. Therefore, a patient may visit a medical facility after suspecting that they would be suffering from pneumonia based on signs and symptoms they may be exhibiting.
Types Of Pneumonia
There are two types of pneumonia: Community-acquired pneumonia (CAP) and hospital-acquired pneumonia (HAP), also known as nosocomial pneumonia.
Pneumonia can also be grouped according to its location and radiologic appearance: Bronchopneumonia involves the terminal bronchioles and alveoli, reticular pneumonia involves an inflammatory response within lung tissue surrounding the air spaces or vascular structures, alveolar pneumonia involves the accumulation of fluid or pus in the lung’s distal air spaces, necrotizing pneumonia causes the death of a portion of lung tissue surrounded by a viable tissue.
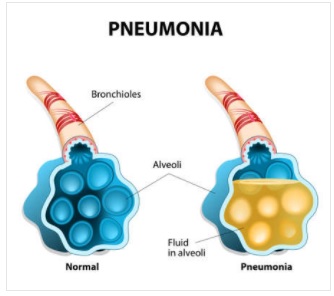
Lastly, pneumonia can be classified according to its microbiologic etiology. This means that that the infection can be viral, bacterial, fungal, protozoan, etc. A nurse needs to identify the different types of pneumonia’s distinctive signs and symptoms to make a proper diagnosis.
Signs and Symptoms Of Pneumonia

The distinctive signs and symptoms of pneumonia include coughing, sputum production, severe chest pains, shaking chills, rapid shallow breathing, fever, and shortness of breath. To arrive at a diagnosis, several processes and procedures are carried out.
First, assessing the patient’s medical history is carried out to see whether the patient has suffered from any other respiratory infections or is suffering from a chronic disease. Respiratory assessments are also done every four hours that include physical examinations and ABG measurements.
The results acquired from these assessments are vital in determining the type of pneumonia the patient may be suffering from.
Nursing Diagnosis For Pneumonia
The most common nursing diagnosis for pneumonia is ineffective airway clearance. This diagnosis is associated with excessive secretions and ineffective cough or otherwise known as non-productive coughing. The ineffective airway clearance resulted from inflammation and increased secretion making it impossible to maintain a patent airway.
Apart from the ineffective airway clearance, a patient suffering from pneumonia may also experience
- tracheal,
- bronchial inflammation,
- edema formation,
- increased sputum production,
- pleuritic pain,
- decreased energy,
- fatigue, and aspiration
The defining characteristics that will guide the nurse to conclude that the patient has an ineffective airway clearance include: changes in rate and depth of respiration, abnormal breath sounds, use of accessory muscles, ineffective cough, hypoxemia and infiltrates seen on x-ray film.
Characteristics
On studying the patient and observing the specified characteristics, the nurse further observes the patient, seeking to identify specific outcomes. This is important to help the nurse make the final diagnosis and conclude that the patient is suffering from pneumonia.
These are the most common desired outcomes for ineffective airway clearance secondary to pneumonia. These outcomes include: the patient may exhibit the extreme desire to achieve airway clearance, the patient may also continue trying to maintain a patent airway with breath sounds clearing, absence of dyspnea, cyanosis, and effectively clearing secretions.
These are the final characteristics that help a nurse fully diagnose a patient with pneumonia.
Pneumonia Diagnosis
The diagnosis process also involves nursing interventions that include further assessment of the patient’s assessment, even after being fully diagnosed with pneumonia.
These assessments include:
- Assessing the rate, rhythm, and depth of respiration, chest movement, and use of accessory muscles. This is because shallow respirations and asymmetric chest movements are usually associated with discomfort of moving chest wall and fluid in the lungs due to compensatory response to airway destruction.
- Assess cough effectiveness and effectiveness and productivity. This is because coughing is the most effective way to get rid of secretions. Pneumonia may cause thick and tenacious secretions to patients.
- Observe the sputum color, viscosity, and odor and report the changes. Changes in sputum characteristics may be characterized by an indication that the patient has an infection. Discolored sputum or one that has odor may increase airway resistance and may require further intervention.
- Encourage ambulation. This helps mobilize secretions and helps in reducing atelectasis.
- Lastly, administer medications as indicated and advise the patient to take the prescribed medicine. If the patient’s situation is persisting even with though with the medication, use humidified oxygen or humidifier at the bedside.
These assessments are important to the nurse in that they ensure that a proper diagnosis was made and that proper treatment was issued to the patient.
Other related nursing diagnoses commonly associated with pneumonia that a nurse can use include impaired dentition. This is associated with dietary habits, poor oral hygiene, chronic vomiting, erosion of tooth enamel, multiple carries, and abraded teeth.
The other diagnosis is impaired oral mucous membrane. This is associated with breathing through the mouth, malnutrition or vitamin deficiency, chronic vomiting, swollen salivary glands, and sore mouth and throat reports.
Conclusion
pneumonia is a disease that is life-threatening and therefore demands urgent medical assistance. If not, a patient exhibiting signs and symptoms associated with pneumonia may die. Therefore, a proper diagnosis and treatment of the disease are highly essential.
Proper care is needed while handling pneumonia patients is also encouraged as the disease is airborne.
References
Doenges, M. E., Moorhouse, M. F., & Murr, A. C. (2016). Nursing diagnosis manual: Planning, individualizing, and documenting client care. FA Davis.
Hollaar, V. R., van der Putten, G. J., van der Maarel-Wierink, C. D., Bronkhorst, E. M., de Swart, B. J., de Baat, C., & Creugers, N. H. (2017). Nursing home-acquired pneumonia, dysphagia and associated diseases in nursing home residents: a retrospective, cross-sectional study. Geriatric Nursing, 38(5), 437-441.
Rowe, T., Eure, T., Stone, N., Thompson, N., Anttila, A., Dumyati, G., … & Kainer, M. (2020). Improving Surveillance of Pneumonia in Nursing Homes. Infection Control & Hospital Epidemiology, 41(S1), s290-s291.
van der Maaden, T., van der Steen, J. T., de Vet, H. C., Hertogh, C. M., & Koopmans, R. T. (2016). Prospective observations of discomfort, pain, and dyspnea in nursing home residents with dementia and pneumonia. Journal of the American Medical Directors Association, 17(2), 128-135.

1 comment
[…] Read our popular article " What is the nursing diagnosis for pneumonia" […]
Comments are closed.